HUV, HUVS, and NUV are the three subtypes of Urticarial Vasculitis.
Urticarial Vasculitis is a form of cutaneous vasculitis characterised by inflammation of the small blood vessels. All three subtypes are defined by a measure of the “complement” levels in the blood. The complement system is a set of proteins that contribute to and amplify immune responses. They play a role in some, but not all, autoimmune disorders including some forms of Urticarial Vasculitis.
Normocomplementemic Urticarial Vasculitis (NUV)
NUV is diagnosed where a patient has the main symptoms of Urticarial Vasculitis combined with normal levels of C1q complements. NUV is generally the least severe form of Urticarial Vasculitis. It is less likely to be associated with any other symptoms.
Hypocomplementemic Urticarial Vasculitis (HUV)
HUV is diagnosed where the patient has the main symptoms of Urticarial Vasculitis combined with lower than normal levels of C1q complements and raised levels of anti-C1q antibodies (antibodies that attack the C1q complements). HUV is a more severe form of Urticarial Vasculitis and is likely to include symptoms such as purple or dark red spots or rash on the skin (a typical vasculitic rash); arthritic joint pain; breathing difficulties such as asthma, and stomach pains. Some regard HUV as a form of SLE (Lupus), although HUV patients usually test Anti-Nuclear Antibody (ANA) negative instead of the normal positive result for Lupus patients.
Hypocomplementemic Urticarial Vasculitis Syndrome (HUVS)
HUVS is a very rare and severe form of Urticarial Vasculitis. HUVS patients have more extensive complement abnormalities (low circulating 3rd and 4th complement components). As well as the symptoms of HUV, patients will suffer from systemic problems such as: episcleritis or uveitis (bloodshot or inflamed eyes) (found in 30 per cent of patients); mild glomerulonephritis (kidney disease); pleuritis (inflammation of the membrane surrounding the lungs); angioedema (swelling of the tissues under the skin) (found in 50 per cent of patients); Chronic Obstructive Pulmonary Disease (COPD) (breathing difficulties) (found in 50 per cent of patients), and cardiac involvement such as myocardial infarction (heart attack)
Who are affected?
NUV is most common between the ages of 30-40 and is found in women more than men. HUV and HUVS are almost exclusively found in women.
What is the aetiology (cause)?
The cause of Urticarial Vasculitis is not known in 50 per cent of cases. However it can be associated with or triggered by autoimmune/connective tissue diseases like Systemic Lupus Erythematosus (SLE or simply Lupus) Rheumatoid Arthritis, or occur in the context of a systemic vasculitis syndrome, such as Churg Strauss syndrome (Eosinophillic Granulomatosis with Polyangiitis); infections or viruses such as hepatitis; a reaction to certain drugs such as ACE inhibitors; certain types of diuretics; penicillin and Non-Steroidal Anti-Inflammatory Drugs (NSAIDs); cancer; and Glandular problems, such as Graves’ Disease (overactive thyroid).
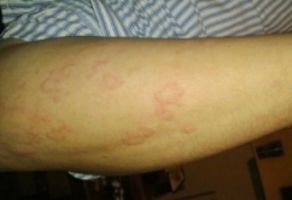
What are the symptoms?
The main symptom is a recurring urticarial (“stinging nettle”) rash that lasts for longer than 24 hours and “burns” rather than “itches”, leaving marks behind on the skin when it clears.
Diagnosis
As in other types of vasculitis, diagnosis will depend on the doctor recognising the pattern of symptoms and examination findings. Blood is commonly taken to test for raised levels of “C-reactive protein” (CRP) and “Erythrocyte Sedimentation Rate” (ESR) which indicate inflammation in the body. Skin and kidney biopsies may also be taken to confirm the diagnosis.
Testing for C1q, anti-C1q, C3 and C4 complement components is essential to determine the type of Urticarial Vasculitis.
Tests may also be done for Anti-Nuclear Antibody (ANA) levels (which are positive in 30 to 50 per cent of patients), and Anti ds-DNA levels may also be positive.
Treatment
Milder cases of Urticarial Vasculitis may simply be treated with antihistamines and NSAIDs such as Ibuprofen. Corticosteroids such as Prednisolone might be used for more persistent cases. However for the more severe forms of Urticarial Vasculitis, steroids such as Prednisolone are usually prescribed to reduce inflammation as well as immunosuppressants such as Azathioprine, Cyclophosphamide or Mycophenolate Mofetil (CellCept).
In cases where a patient is unresponsive to treatment, intravenous immunoglobulin and anti-cytokine monoclonal antibodies or rituximab may have a role.
If the disease is very severe large doses of Methylprednisolone or Plasmapheresis (plasma exchange) may also be given. When the disease becomes quiet less toxic drugs are used to keep control and these include: Azathioprine, Methotrexate and Mycophenolate Mofetil usually in combination with low dose prednisolone.
Drugs and Side Effects
For information on the main drugs prescribed for Urticarial Vasculitis see:
For information on other drugs used in the treatment of vasculitis see Glossary of drugs and side effects.
Treatments – Procedures
Plasma exchange or plasmapheresis
This treatment is sometimes used in patients with severe vasculitis where antibodies in the blood are thought to be important in causing the disease. The treatment involves removing antibodies from the blood using a machine and returning the “cleaned” blood back to the patient. The treatment may necessitate giving blood products to the patient including plasma, albumin or immunoglobulin. It may also involve giving drugs to thin the blood and prevent it clotting in the machine.
For information on plasma exchange:
Prognosis
The overall prognosis in Urticarial Vasculitis depends on the severity of the disease and the amount of damage that has been done to organs, especially the lungs. The main risk to patients appears to be Chronic Obstructive Pulmonary Disease (COPD).
Smoking is a major risk factor for fatal lung disease in HUVS and smokers should seek help to give up as soon as possible.
Key Points
- The systemic HUVS type of Urticarial Vasculitis is a very rare form of the disease
- The main symptom is a recurring urticarial (“stinging nettle”) rash
- The levels of C1q complements in the blood are a significant indicator for diagnosis and treatment
- Treatment depends upon the severity of the disease
Related Vasculitis Articles
- Fertility and Vasculitis – Dr David Jayne
- Vasculitis Paediatric Guidelines 2012 – Dr Helen Foster & Dr Paul Brogan, Oxford University Press
Further reading
- Hypocomplementemic Urticarial Vasculitis Syndrome – Wisnieski JJ, Baer AN et al
- Vasculitis: Approach to diagnosis and therapy – Aparna Palit, Arun C Inamadar
- Hypocomplementemic Urticarial Vasculitis Syndrome – An Interdisciplinary Challenge – Wolfgang Grotz, Hideo A Baba et al
- Hypocomplementemic Urticarial Vasculitis Syndrome – A Case Report and Literature Review – Andrew Buck, Jim Christensen, and Morgan McCarty
