What is Giant Cell Arteritis/Temporal Arteritis?
GCA is a disease characterised by inflammation of large and medium sized blood vessels. An alternative name for this condition is “Temporal Arteritis” as the blood vessels in the temple area of the head (sides of the forehead) are commonly affected. The giant cells referred to are specific collections of immune system cells seen in the areas of inflammation if a biopsy is performed.
Who are affected?
This condition is one of the commonest forms of vasculitis, affecting one or two persons per 10,000 people in the UK. It is more commonly seen in older patients and is seldom diagnosed below the age of 50.
What is the aetiology (cause)?
The cause of Giant Cell Arteritis/Temporal Arteritis is not yet known.
What are the symptoms?
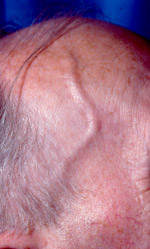
Symptoms of fatigue, loss of appetite, weight loss and fever are often found. Headache, with pain and tenderness over the temples, is a prominent feature of this disease due to inflammation of the temporal arteries. GCA is closely associated with the Polymyalgia Rheumatica Syndrome which causes general weakness, pain and stiffness in muscles and joints. The weakness in the muscles can be quite debilitating and typically affects the upper arms and legs. Simple tasks such as brushing the hair, cooking, gardening, getting up and out of chairs or beds and walking may become difficult.
As this condition affects the main blood vessels supplying parts of the body, a reduction in the blood and oxygen supply (ischaemia) to different organs can result. This can lead to a variety of symptoms. A classic symptom of this condition is pain in the tongue or jaw when eating (jaw claudication). Reduction of the blood supply to the brain can cause a stroke. Reduction in the blood supply to the eyes can lead to blurred vision, or in some patients, blindness.
Making a diagnosis
As with most types of vasculitis there is no one test that will give the diagnosis. The diagnosis is usually made because the doctor recognises the typical collection of symptoms and clinical signs. Blood tests for inflammation (ESR – erythrocyte sedimentation rate; CRP – C-reactive protein; plasma viscosity) will usually be high indicating inflammation but these are not specific and can be raised in any type of vasculitis, many infections and other types of inflammatory disease. If the temporal arteries are involved (located at the sides of the forehead over the temples) then a biopsy may be performed. If the biopsy shows inflammation this will help to confirm the diagnosis. Unfortunately a biopsy without inflammation does not exclude the diagnosis. Sometimes an ultra sound scan of the arteries is used instead of a biopsy.
Treatment
The two aims of treatment are to relieve patient’s symptoms and prevent damage to organs (especially the eyes) due to reduced blood supply. High dose oral steroids (Prednisolone) are usually given and the dose is reduced slowly over months, using the ESR marker as a guide to response. Treatment with steroids is usually given for at least one or two years.
In some patients with resistant or problematic disease other drugs are sometimes used such as methotrexate, Azathioprine or antibody therapy such as infliximab. While some patients may respond well to these drugs there is no current evidence that they are effective in all patients.
Drugs and Side effects
For information on the main drugs prescribed for Giant Cell Arteritis see:
For information on other drugs used in the treatment of vasculitis see Glossary of drugs and side effects.
Prognosis
There is a relapse rate of about 50 per cent. Withdrawal of the steroids can lead to a relapse of the symptoms. In such cases the steroid is re-started and it is often sufficient to induce remission. The steroid dose can again be reduced. In most relapsed cases the patient will be maintained on a small maintenance dose of steroids indefinitely. The prognosis is good with correct and early diagnosis and treatment.
Key Points
- GCA is one of the commonest forms of vasculitis
- Symptoms include headache and jaw claudication (cramping pain)
- Temporal artery biopsy or ultrasound scan may help confirm the diagnosis
- Damage to the eyes is usually the most serious complication
- Treatment is usually with steroids and may continue for many years.
Related Vasculitis Articles
- Fertility and Vasculitis – Dr David Jayne
- Vasculitis and the Eyes – Dr Catherine Guly
Further reading
- Giant Cell Arteritis: Suspect it, treat it, treat it properly – Alexandra Villa-Forte
- The Treatment of Giant Cell Arteritis – J. Alexander Fraser, Cornelia M. Weyand, et al
- Large Vessel Diseases – Ashima Gulati, Arvind Bagga
- Report – Research into Giant Cell Arteritis – Science Daily – 17 Jan 2014
Useful links
Our Useful Vasculitis Links page contains contact details for organisations offering help and support for patients with Giant Cell Arteritis, Polymyalgia Rheumatica and other vasculitis diseases.
