Dr Alina Casian (Nephrology)
Thomas and Guys Hospital, London
Supported by
Professor David D’Cruz, Consultant Rheumatologist (Lupus & Connective Tissue Disease)
Thomas & Guys Hospital, London
February 2016
What is Relapsing Polychondritis?
Relapsing polychondritis is a rare disease that presents with inflammation of cartilage in several parts of the body, usually affecting the ears, nose, throat and lungs. It occurs most often in people in their 50s or 60s and is more common in people with white/Caucasian ancestry.
What is the aetiology (cause)?
The cause is not clear; it is thought that polychondritis is an autoimmune disease, in which the body’s defence (immune system) attacks its own cartilage. Polychondritis does not appear to run in families, although some people may have genes that increase their risk of developing the disease. It sometimes occurs in patients with other autoimmune diseases, including rheumatoid arthritis, lupus or vasculitis (inflammation of blood vessels).
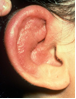
What are the symptoms?
Polychondritis is a systemic (body-wide) illness. Common initial symptoms are pain and swelling in the ears that may become red.
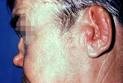
Eventually floppy ears, loss of hearing, ear infections, balance disturbances with vomiting can occur. Throat pain, hoarse voice and speech problems may also appear. The nose could feel blocked and more flat (‘saddle nose’).
Joint pains and swelling, tiredness and weight loss are other common symptoms in RP; fever is often present during flares of the disease.
RP may also cause stridor (high-pitched sound during breathing) and shortness of breath due to damage of the cartilages from the windpipe and ribs. Damage to the airways increases the risks of chest infections.
The disease may flare from time to time but remain under control in between, or it may cause persistent symptoms and, gradually, more damage to organs. The type, severity and frequency of RP symptoms varies between people and with time.
Other, more rare symptoms include: eye inflammation, leaky heart valves, kidney disease, nerve problems, skin rash.
Diagnosis
The diagnosis of RP is frequently made late, because its various symptoms may be similar to and mistaken for other, more common, diseases. Patients may be diagnosed with polychondritis when relevant symptoms are present (as below) and a biopsy supports the diagnosis.
The diagnosis can usually be confirmed by biopsy of an inflamed tissue, removing a small piece and examining it under a microscope. Sometimes, the biopsy may not be informative or does not need to be done because the doctor is sure of the diagnosis.
No single blood test can give the diagnosis. Lung function tests and computed tomography (CT) scan pictures may be done to help clarify the severity of disease.
If a biopsy is not obtained, the diagnosis is still likely when a person has at least 3 of the following:
- Inflammation of cartilage in both ears (excluding the soft lower earlobe)
- Pain and swelling in several joints
- Inflammation of the nose cartilage
- Eye inflammation
- Inflammation of the cartilage in the windpipe or throat
- A type of hearing loss (called sensorineural hearing loss), tinnitus (ringing sound in the ears), a sensation of spinning (vertigo)
Expected Duration
Polychondritis is a chronic (long-term) disease, although medications can frequently keep it under control and improve symptoms. Sometimes, RP becomes “quiet” (in remission) temporarily.
Treatment
The best treatment for this rare disease is unclear because it is difficult to find a sufficient number of patients to take part in research studies. Treatment depends on which organs in the body are affected and how seriously.
Although RP does not have a complete cure so far, it is often well controlled with medication such as methotrexate, and steroids for acute flares.
For less serious disease, affecting only the joints or skin, nonsteroidal anti-inflammatory drugs, painkillers, dapsone or steroids may be used. For more severe RP, medicines that dampen the immune system (such as methotrexate, azathioprine, cyclosporin or cyclophosphamide) are also given.
Recently, other medicines (including infliximab, adalimumab, etanercept, abatacept, leflunomide, mycophenolate mofetil, tocilizumab or rituximab) were shown to improve severe polychondritis in a few people with RP. However, because of the small numbers of patients, the role of these treatments remains uncertain.
Repair of the windpipe or stenting (insertion of a small plastic tube to keep the airway open) are other useful options in some cases. Antibiotic treatment can save lives when the patients also have a chest infection.
Prognosis
The outcomes for people with polychondritis vary a lot. People whose lungs are affected may have a shorter life span. However, disease which is more mild or responds quickly to treatment can have an excellent prognosis.
Despite the fact that many patients have some problems with hearing, eyesight or breathing, RP is often chronic but tolerable.
Key Points
- Relapsing polychondritis is a rare autoimmune disease that causes inflammation of the cartilages
- RP may be mistaken for more common conditions and thus diagnosed late
- Treatment depends on the severity of the disease
- Many patients respond well to standard treatment with medicines that dampen the immune system (such as methotrexate) and steroids
- The disease may flare again after the initial treatment
- Future studies including more patients are needed to clarify the best treatment
Other Relapsing Polychondritis Patient Information
National Organization for Rare Disorders (NORD) – USA
http://www.rarediseases.org/
Phone: 00 1 800 999-6673
Monday-Thursday: 0900-2000 EST, Friday: 0900-1800 EST (5 hours after GMT)
Relapsing Polychondritis Support Group (UK) (started in 1987)
https://groups.yahoo.com/neo/groups/relapsingpolychondritisUK/info
Email: [email protected]
