The first part of this story was written in early 2012 for the Vasculitis UK Spring Newsletter/Journal.
I was born in October 1982 at a hospital that later would diagnose me with Wegener Granulomatosis. I grew up, as most kids do, playing out and riding my bike. I also had rally cars around me as my dad was into rallying and some of the local motor club cars were in the garage on the side of my house. At 12 I was cycling competitively mainly time trialing at 10 to 25 mile. By 17 I started training as a motor technician and I also started racing 100cc race karts which I raced for a few years. I became a fully qualified motor technician in 2003 but then had a small break from cars and worked at the Cumberland pencil mill. I also took up rallying with my dad coming out of retirement to navigate for me.
During summer 2010 I just didn’t feel myself, always tired and feeling ill. By October 2010, whilst out rallying, I felt so ill and needed help out of the car at end of the day. I saw the GP next day and was told it was “just the flu”.
The following week I was feeling even worse. My sinuses where causing problems. Sinusitis was diagnosed and antibiotics prescribed. I returned to the GP feeling worse and she went through all my symptoms: pain from my sinuses, coughing up blood, bad nose bleeds, flu-like feeling, night sweats, sickness, and weight loss (3 stones).
Blood tests were ordered, but later that week I was unable to get out of bed, was very weak and stared getting chest pains. An emergency appointment was arranged and they suspected I had pneumonia. However my blood had way too many white cells and very few red cells. I was admitted to Whitehaven Hospital. I underwent lung biopsies internal with a camera and external. Unfortunately they punctured my right lung and so a chest drain was fitted. The biopsy confirmed what they suspected – Wegener’s Granulomatosis. I started chemotherapy two weeks before Christmas.

I returned to work after four months having to take a week off every month for my chemo. This continued until May. I also started rallying again in the March and came second in class in the ANECCC SG Petch Rally Championship in 2011.
Since diagnosis in 2010 I am continuing to learn to live with WG and it has been a bumpy ride. I don’t like to admit it but I am ill at times, and sometimes it’s a struggle. BUT IT WILL NOT WIN and I will fight on, hopefully into old age.
Andrew continues his story (March 2013) with details about his tear duct problem and gives a truthful account of his recent operation
Starting at the beginning. I had been having problems for a long time. Initially these were intermittent but later becoming almost constant so that my eyes would water, stop then restart. This fluid would collect but wouldn’t drain away and I would get a swelling in the lacrimal sac which would then cover my eye. This was all caused by the damage to my senus caused by my WG.
My doctors offered me a solution – an operation – which I agreed to, without fully thinking it all through. But I just wanted an improvement and was willing to try. It was undertaken as a joint venture between the ENT and ophthalmology departments.
There are a few ways to improve the watering but only one is worth trying with with WG and the following is my story.
I basically have had what are known as Lester Jones tubes fitted (lacrimal bypass tubes). The tube is a Pyrex glass tube that is flared on both ends to help it collect fluid, to hold it in position and to offer a point for the tears to drain away from the corner of your eye to inside the nose. I am sure I don’t need to go into greart detail but the tear duct is a drain for tears into the nose. Tears are made by the lacrimal gland and the tears are used for lubricating and cleaning the eye. I only know the basics. Tears are not, as someone suggested to me, only for crying!
Prior to the operation I had to use nose drops twice a day. Getting them to the point required involved hanging off my bed upside down to enable them to run to the exact positin. This manoeuvre had to be done twice a day for a month. After a postponed operation date I finally attended the day surgery ward and from there to theatre. Two hours later I remember coming round in the recovery ward with it all done.
So what did it involve? Well from what I understand from the doctors, they carry out most of the operation from inside your nose using a laser. This involves creating a small passage to insert the Pyrex tube into, a small needle to gauge the length required and a plastic tube which is fitted over the Pyrex tube. All is then stitched to hold it in place until the flesh heels. Then the plastic tube is removed. This procedure is repeated on both sides.
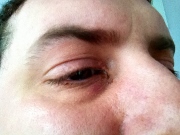
I suffered from bad nose bleeds but I was aware this could happen. Unfortunately I developed an infection which resulted in heavy nasal discharge. Being unable to blow my nose I found that I could wash it out with a saline rinse and that helped.
Things didn’t improve. Two days later my face swelled up as did my tonsils and my tongue. However this only lasted a few days. After that any pain could be controlled with pain killers. The pain eased as the swelling went down and as the tubes settled into their new permanent position.
Two weeks later it was time for the stitches to come out. Unfortunately only one side was working satisfactorily, but I was having problems (watering) with the other and it was quite uncomfortable. It was decided to wait a little longer before proceeding and things have improved although I can at times still feel the tubes. Time will tell how well they work and if they have made a permanent improvement.
So would I have it done if I’d asked the questions and been aware of the positives and negatives? Well………. I think I will let you decide. However the long term positive is: improved watering by a new way of draining into the nose.
The negatives: the tubes can fall out or move, they block regularly and require a saline sinus rinse every day sometimes more often , they can dig into the eye and are uncomfortable; and blowing your nose and mucus coming up the tube into the eye isn’t pleasant.
Ok there are more negatives, but I would like to stress that, like all things related to WG, these negatives might not happen to everybody. I would suggest that if you are contemplating this operation you should discuss it fully with your ENT and ophthalmology department specialist. They will advise you. However, remember to ask the questions.
I hope that this has been of some help.
