How to navigate life with a subglottic stenosis.
By Charlie Harper
It is easy forget that we are always breathing, the gentle flow of air in and out of the lungs has inspired numerous types of mediation and relaxation practices. But for GPA patients living with a subglottic stenosis, every breath can be a struggle.
My name is Charlie, I am 28 and live in Oxford. I want to tell my story and what I have learnt through living with a subglottic stenosis. I hope my experiences and “top tips” can help others navigate life with such a debilitating and scary condition.
First, what is a subglottic stenosis? A subglottic stenosis refers to the narrowing of the windpipe just below the vocal cords. It starts with inflammation of small blood vessels in the windpipe, with inflammatory tissue building up and eventually turning into thick scar tissue. Around one in ten people with GPA develop a subglottic stenosis. With treatment usually a combination of increasing steroids/immunosuppressants and/or surgical dilations of the throat. The symptoms for patients are often scary and debilitating, with many describing feelings of being “strangled” and “always trying to catch their breath”. Unfortunately, this manifestation of GPA is not often talked about, and I would like to share my story so others a more aware of this disease.
My story starts back in the summer of 2019, I had been diagnosed (with GPA) in March of that year and was tapering off my steroids as the disease was believed to be under control. Slowly over many weeks my breathing started to get noisier and felt like a lump was stuck in my throat. After this got worse, I ended up in A&E with breathing difficulties. ENT diagnosed the subglottic stenosis quickly and Rheumatology were able to act quickly to up my steroids and start me on cyclophosphamide (as previously as I was on Rituximab only). Soon after this I went into surgery, with ENT dilating (stretching) my windpipe and providing some small laser cuts around the area. The surgery really helped short-term and allowed me to breath normally again.
Here are my tips on managing life with a stenosis:
- Have a direct email/telephone number of your local ENT team. If your breathing worsens, you don’t want to be stuck in A&E for hours trying to explain to the receptionist/nurse why you are there and who you need to see.
- Invest in a good nebulizer. Using a nebulizer with saline solution helped me manage my symptoms at home.
- Find your most comfortable position. It is important you find a place/position at home you feel most comfortable breathing (for example I found I could breathe easiest on my side lying down).
- It’s normal to be noisy. When my stenosis was particularly bad, my breathing sounded like a hiss and was most noticeable around others less familiar with my health. But it is important to remember this is okay and normal: if it is something you feel self-conscious about then spend time with those you feel most comfortable around.
- Rest your voice. Speaking can become exhausting, as you are trying to push air out of a very small hole in your throat. Try to talk in short bursts (15-20 mins) then have quiet times in the day to rest it.
Unfortunately, my story does not stop there.
Over several months my stenosis continued to get worse, and surgical treatment was only effective for a few weeks. After some very difficult days, I ended up in A&E again in November 2019 with little ability to breathe. I was given adrenaline and then taken into the operating theatre to undergo an insertion of a tube in my throat (called a tracheostomy). Fortunately, this was not a surprise for me as my surgeon had already warned me this would be the last resort.
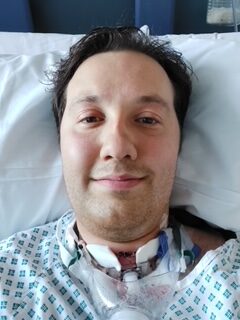
After the surgery, the experience of waking up is quite scary. I was not able to speak as they had blocked my upper airway, I could not move my neck, I had a feeding tube, and lost all independence for a short period. Without doubt, one of the worst moments that I have experienced with GPA. But I was able to recover quickly, and within a few weeks I was swallowing and speaking again, with nurses teaching me how to manage my own tracheostomy at home.
Here are my tips on managing life with a tracheostomy:
- Get in contact straight away with the private medical supplier who will send you tracheostomy supplies free of charge (mine is called Atos Medical).
- Learn as much as you can while in hospital about cleaning and looking after the device. Nurses are a great place to start, and they are happy to go over things as many times as you need.
- It does get better. When you leave hospital, it will be challenging to look after, and the stoma will take a while to heal. A few months later and all the inflammation will have died down and living with the tracheostomy is far easier.
- Keep an eye on the weather. Breathing can be challenging on days where the temperature is particularly cold or wet. The summers tend to be far easier than the winter months.
- Build confidence in leaving the house. With a whole new addition to your day-to-day life, practice with a loved one leaving the house, over time gaining confidence to do it by yourself.
Soon after having the tracheostomy in place, I lost my voice completely due to the airway fully closing. Me and my wife had to negotiate communicating, often mouthing words, or using hand gestures. Throughout this period my daughter Heidi was born, and the new parent experience had to go hand in hand with managing without a voice. After further rounds of cyclophosphamide and further dilations, I was finally able to gain my voice again and smell my daughter for the first time. We recorded the first time I was able to speak to her, a magical moment for us all. We were worried that she would grab and damage the device, but after lots of repetition she learnt it to be normal (like someone might wear glasses).
A year on from these life changing events and I still live with a tracheostomy; it is so normal now that I forget I have it. Life remains challenging with it but is far sweeter for me with a wonderful daughter and wife. Soon I will be undergoing a full resection (reconstruction) of my throat in London, and we hope that this may be my final airway procedure, with the tracheostomy tube also being removed.
There is no doubt that this whole journal has been incredibly hard, with many points where I lost hope. But the value of community (family/friends/nurses/doctors) cannot be understated, I would not be where I am today without each one of these individuals. So, I want to say THANK YOU.

